You moved abroad six months ago, and your hair is falling out in clumps. You’re waking up at 3 AM with your mind racing about work deadlines, visa renewals, and whether you made the right choice leaving home. Your shower drain clogs weekly now. And everyone keeps telling you it’s just stress, as if that explains why you’re losing hair you spent years growing.
This article contains affiliate links. See our affiliate disclosure for details.
Here’s what they’re not telling you: the connection between stress and hair loss isn’t vague or psychological. It’s biochemical, measurable, and directly linked to cortisol dysregulation. When you’re living in a state of chronic stress (which most expats are, whether they admit it or not), your body prioritizes survival over non-essential functions like hair growth. The result is a specific type of hair loss called telogen effluvium, and it typically shows up 2-3 months after your stress levels spike.
The expat experience is uniquely positioned to trigger this cascade. You’re dealing with cultural adjustment, language barriers, environmental factors like hard water, changeed sleep schedules, and the constant low-level anxiety of being far from your support system. Your body interprets all of this as threat. And when your body feels threatened, it shuts down hair follicles to conserve resources.
Medically reviewed by Dr. Layla Hassan, Trichologist. The good news is that stress-induced hair loss is reversible if you address the root cause: your dysregulated cortisol rhythm. This isn’t about meditation apps or bubble baths. It’s about understanding the specific mechanisms linking sleep deprivation, cortisol improvion, and follicle dysfunction, then implementing targeted interventions that actually work.
The Cortisol-Hair Loss Mechanism: What’s Actually Happening
Cortisol is your primary stress hormone, and under normal circumstances, it follows a predictable daily rhythm. It peaks in the early morning (around 8 AM) to help you wake up, then gradually declines throughout the day, reaching its lowest point around midnight. This pattern is called your circadian cortisol rhythm, and it’s essential for healthy hair growth.
When you’re under chronic stress, this rhythm gets changeed. A 2019 study published in the International Journal of Molecular Sciences found that sustained cortisol improvion directly impacts hair follicle cycling by shortening the anagen (growth) phase and prematurely pushing follicles into the telogen (shedding) phase. Normally, about 85-90% of your hair follicles are in active growth at any given time. Under chronic stress, that percentage can drop to 50-60%, with the displaced follicles entering premature shedding.
The mechanism works like this: improved cortisol triggers the release of substance P and other neuropeptides in the hair follicle, creating local inflammation. This inflammation changes the delicate signaling pathways that keep follicles in the growth phase. At the same time, cortisol suppresses the production of growth factors like IGF-1 (insulin-like growth factor 1) and VEGF (vascular endothelial growth factor), both of which are critical for maintaining blood flow to the scalp and supporting follicle function.
For expats specifically, the stress isn’t just psychological. You’re dealing with circadian changeion from time zone changes, vitamin D dysregulation despite sun exposure, dietary changes that affect nutrient availability, and often significant sleep deprivation. All of these factors independently improve cortisol, and their combined effect is what triggers the hair loss you’re seeing 8-12 weeks later.
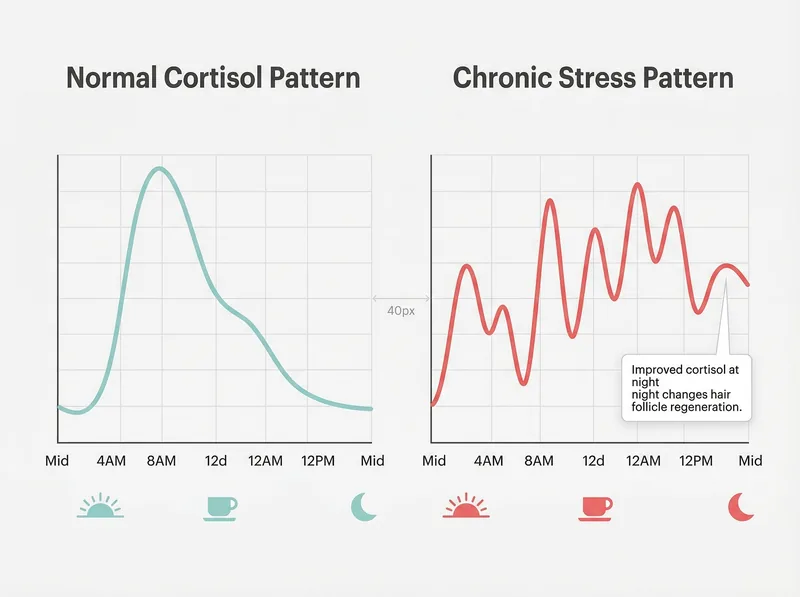 How chronic stress changes your natural cortisol rhythm and impacts hair growth cycles
How chronic stress changes your natural cortisol rhythm and impacts hair growth cycles
Telogen Effluvium: The Clinical Pattern of Stress Hair Loss
Telogen effluvium is the medical term for diffuse hair shedding triggered by a systemic stressor. Unlike androgenetic alopecia (pattern hair loss), which is genetic and progressive, telogen effluvium is temporary and reversible once you address the underlying trigger. But that doesn’t make it any less distressing when you’re losing 200-300 hairs per day instead of the normal 50-100.
The timeline is consistent and predictable. Research in Dermatology Practical & Conceptual shows that telogen effluvium typically manifests 2-3 months after the stressor begins. This delay happens because hair doesn’t fall out immediately when a follicle enters telogen. The hair shaft remains anchored in the follicle for the full 3-4 month telogen phase before it’s pushed out by a new hair growing underneath (or in chronic cases, by nothing at all).
For expats, this means the hair loss you’re experiencing now is likely related to stress from several months ago, possibly around the time of your move or a significant work deadline. The shedding can continue for 6-9 months if the stressor remains unresolved, which is why so many expat women report that their hair loss doesn’t stop even after they’ve “adjusted” to their new location. The stress hasn’t actually resolved. It’s just become normalized.
The clinical presentation is diffuse thinning across the entire scalp, often most noticeable at the crown and along the part line. You’ll see increased shedding when you wash your hair, run your fingers through it, or brush it. The individual hairs that fall out typically have a small white bulb at the root (the telogen club hair), confirming they’ve completed their growth cycle and entered shedding phase. If you’re also seeing broken hairs without the white bulb, that suggests additional damage from environmental factors like hard water mineral buildup.
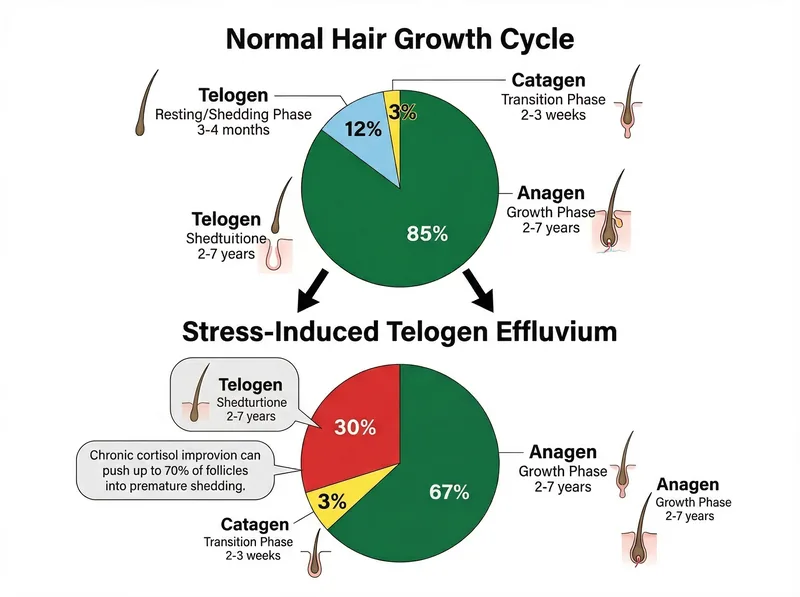 Stress-induced telogen effluvium: when cortisol pushes hair follicles into premature shedding
Stress-induced telogen effluvium: when cortisol pushes hair follicles into premature shedding
Sleep Deprivation: The Hidden Cortisol Amplifier
If cortisol dysregulation is the mechanism, sleep deprivation is the amplifier. A 2017 study in the journal Sleep found that even a single night of sleep restriction (4-5 hours) increases next-day cortisol levels by 37% and changes the normal morning cortisol peak, causing it to remain improved throughout the day and into the evening.
For expats dealing with jet lag, shift work, or the constant low-level anxiety that makes it hard to fall asleep in an unfamiliar environment, this becomes a chronic issue. You’re not just stressed. You’re stressed and sleep-deprived, which means your cortisol rhythm is completely changeed. Instead of the healthy pattern where cortisol drops at night (allowing melatonin to rise and initiate restorative sleep), your cortisol stays improved, suppressing melatonin and making it even harder to sleep. It’s a vicious cycle.
The impact on hair growth is direct and measurable. During deep sleep (stages 3 and 4), your body releases growth hormone, which stimulates cell division in the hair follicle matrix. Growth hormone also counteracts cortisol’s catabolic effects, protecting your follicles from premature shutdown. When you’re not getting adequate deep sleep (which requires 7-9 hours of total sleep time), you’re missing the window for this protective mechanism to function.
Additionally, sleep deprivation impairs your body’s ability to regulate blood sugar, leading to insulin spikes that further improve cortisol. It reduces the production of leptin (the satiety hormone) and increases ghrelin (the hunger hormone), causing you to crave high-glycemic foods that spike blood sugar and trigger more cortisol release. The entire metabolic cascade works against hair growth, and it all stems from inadequate or changeed sleep.
Environmental Stressors in the Gulf: The Compounding Effect
If you’re living in the Gulf region, you’re dealing with additional environmental stressors that amplify the cortisol-hair loss connection. The extreme heat (often 40-50°C in summer) is a physiological stressor that increases cortisol production as your body works to regulate temperature. The high humidity affects sleep quality by making it harder for your body to cool down at night, which is necessary for sleep onset.
The hard water in Gulf countries contains high concentrations of calcium, magnesium, and sometimes heavy metals that create a film on your scalp and hair. This isn’t just cosmetic. The mineral buildup clogs follicles and creates a low-grade inflammatory environment on the scalp, which compounds the inflammation already triggered by improved cortisol. When you’re trying to address stress-induced hair loss, starting with a chelating shampoo like Regrowth+ to remove the mineral barrier is essential before any other treatments can penetrate effectively.
The cultural adjustment of expat life adds another layer. You’re navigating different work expectations, social norms, and often language barriers that require constant cognitive effort. Research from the American Psychological Association shows that chronic cognitive load (the mental effort required to function in an unfamiliar environment) improves baseline cortisol levels by 20-30% compared to operating in your native culture.
The combination of these factors creates a perfect storm for hair loss. You’re physiologically stressed by the environment, psychologically stressed by the adjustment, sleep-deprived from the heat and anxiety, and dealing with water quality that damages your hair shaft while your follicles are already compromised. No single intervention will fix this. You need a complete approach that addresses cortisol regulation, sleep improvation, and environmental protection simultaneously.
 Evidence-based sleep practices that help regulate cortisol and protect your hair growth cycle
Evidence-based sleep practices that help regulate cortisol and protect your hair growth cycle
What Actually Helps: Evidence-Based Cortisol Regulation
The first priority is sleep. Not sleep hygiene tips like “avoid screens before bed” (though that helps). Actual, structural changes to your schedule that prioritize 7-9 hours of sleep in a dark, cool room with consistent bedtimes and wake times. A 2018 study in the Journal of Clinical Endocrinology & Metabolism found that extending sleep from 6 hours to 8 hours per night reduced daytime cortisol levels by 25% within two weeks and restored the normal circadian cortisol rhythm within four weeks.
Magnesium supplementation supports this process. Magnesium glycinate (200-400mg taken 1 hour before bed) enhances GABA activity in the brain, which counteracts cortisol’s stimulating effects and promotes sleep onset. Research shows that magnesium supplementation also reduces inflammation and supports healthy cortisol metabolism, addressing both the sleep changeion and the follicle inflammation simultaneously.
Protein intake matters more than most people realize. Your body needs adequate amino acids to produce the neurotransmitters that regulate cortisol (like serotonin and dopamine) and to build the structural proteins in your hair shaft. Aim for 1.2-1.6g of protein per kilogram of body weight daily, distributed across three meals. A complete supplement stack should include protein improvation alongside targeted nutrients like iron, zinc, and B vitamins that support both stress resilience and hair growth.
Movement helps, but not intense exercise. High-intensity workouts further improve cortisol, which is counterproductive when you’re already dealing with chronic stress. Instead, focus on moderate-intensity activities like walking, swimming, or yoga that lower cortisol while improving insulin sensitivity and supporting healthy sleep. The goal is to move your body enough to regulate blood sugar and reduce systemic inflammation without adding more physiological stress.
Finally, address the environmental factors. Use a chelating shampoo weekly to remove hard water mineral buildup. Install a shower filter if possible (though be realistic about its limitations in Gulf water systems). Protect your hair from heat damage by minimizing blow-drying and heat styling. These interventions won’t fix the cortisol problem, but they prevent additional damage while your body recovers from the stress-induced shedding phase.
Timeline for Recovery: What to Expect
Here’s the reality: if you implement these changes today, you won’t see new hair growth for 3-4 months. That’s how long it takes for follicles to transition out of telogen, re-enter anagen, and produce a hair shaft long enough to be visible. The shedding may continue for another 4-8 weeks as the remaining telogen hairs complete their cycle and fall out.
This delayed timeline is why so many women give up on interventions that are actually working. You’re doing everything right, your cortisol levels are normalizing, your sleep is improving, and your hair is still falling out. It feels like failure. But what’s actually happening is that the hairs currently shedding are the ones that entered telogen 3 months ago, before you started addressing the problem. The follicles that are responding to your interventions are still under the scalp, in early anagen, growing hairs you won’t see for several more weeks.
The first sign of recovery isn’t reduced shedding. It’s the appearance of short, fine “baby hairs” along your hairline and part line. These are the new anagen hairs that started growing 6-8 weeks ago and are now long enough to be visible. You’ll also notice that the hairs falling out start to have longer shafts, indicating they completed more of the anagen phase before entering telogen. These are positive signs that your follicles are responding.
Full recovery typically takes 9-12 months from the point when you address the underlying stressor. By month 6, you should see measurably less shedding and noticeable regrowth. By month 9, the density should be visibly improved. By month 12, most women report that their hair has returned to pre-stress thickness, though the texture may be slightly different (often finer or with more wave pattern) due to the follicle remodeling that occurred during the telogen effluvium episode.
When to See a Healthcare Professional
If you’ve addressed sleep, stress, and environmental factors for 6 months and you’re still experiencing significant shedding (more than 150 hairs per day), it’s time to see a dermatologist or trichologist. Persistent shedding despite intervention suggests there may be an additional underlying cause: thyroid dysfunction, iron deficiency, autoimmune conditions, or androgenetic alopecia occurring alongside the telogen effluvium.
The American Academy of Dermatology recommends complete blood work including complete blood count (CBC), ferritin, thyroid panel (TSH, free T3, free T4), vitamin D, and vitamin B12 for any woman experiencing unexplained hair loss lasting more than 6 months. These tests can identify treatable deficiencies or conditions that are preventing recovery.
You should also seek professional evaluation if you notice sudden, patchy hair loss (rather than diffuse thinning), scalp pain or tenderness, visible scalp inflammation or scaling, or if the hair loss is accompanied by other symptoms like unexplained weight changes, extreme fatigue, or mood changes. These patterns suggest conditions beyond simple telogen effluvium that require medical diagnosis and treatment.
Remember that telogen effluvium is a diagnosis of exclusion. A qualified professional will rule out other causes before confirming that stress and cortisol dysregulation are the primary drivers. Getting this confirmation is valuable because it allows you to focus your interventions with confidence rather than trying random treatments and hoping something works.
References
- The Role of Stress and the Hypothalamic-Pituitary-Adrenal Axis in the Pathogenesis of the Metabolic Syndrome - International Journal of Molecular Sciences
- Telogen Effluvium: A Complete Review - Dermatology Practical & Conceptual
- Sleep Restriction Increases the Risk of Developing Cardiovascular Diseases by Augmenting Proinflammatory Responses - Sleep
- Effects of Sleep Extension on Sleep Duration, Sleepiness, and Blood Pressure - Journal of Clinical Endocrinology & Metabolism
- The Effect of Magnesium Supplementation on Primary Insomnia in Elderly - PubMed
