Three weeks after moving to the Gulf, you wake up with a headache that won’t quit. Your skin feels tight and itchy. Your hair texture has changed completely. You’re exhausted despite sleeping eight hours. And you can’t figure out what you’re doing wrong.
Here’s what no one tells you before you relocate: your body doesn’t just adjust to a new climate. It undergoes significant physiological changes that affect everything from your hydration status to your hormone production. What you’re experiencing isn’t personal failure or poor adaptation. It’s your body working overtime to recalibrate to an entirely different environmental baseline. This article contains affiliate links. See our affiliate disclosure for details.
The transition to extreme heat, low humidity, and hard water creates a cascade of biological responses. Some are immediate. Others take months to fully manifest. Understanding what’s happening beneath the surface and how to support your body through the process makes the difference between struggling through the first year and actually thriving in your new environment.
Key Takeaways
• Your body undergoes measurable physiological changes when relocating to a drastically different climate, affecting hydration, temperature regulation, hormone production, and cellular function
• The adaptation timeline spans 4-6 months, with different body systems adjusting at different rates. Hydration changes occur within days, while full hormonal adaptation can take several months
• Extreme heat increases your baseline fluid needs by 50-100%, and the mineral content in local water directly affects how well your body absorbs and retains that hydration
• Hair loss, skin changes, and sleep changeion during relocation aren’t signs of poor health but normal physiological responses to environmental stress that require specific support strategies
• Strategic supplementation, environmental modifications, and targeted personal care products can significantly accelerate your body’s adaptation and reduce the severity of relocation symptoms
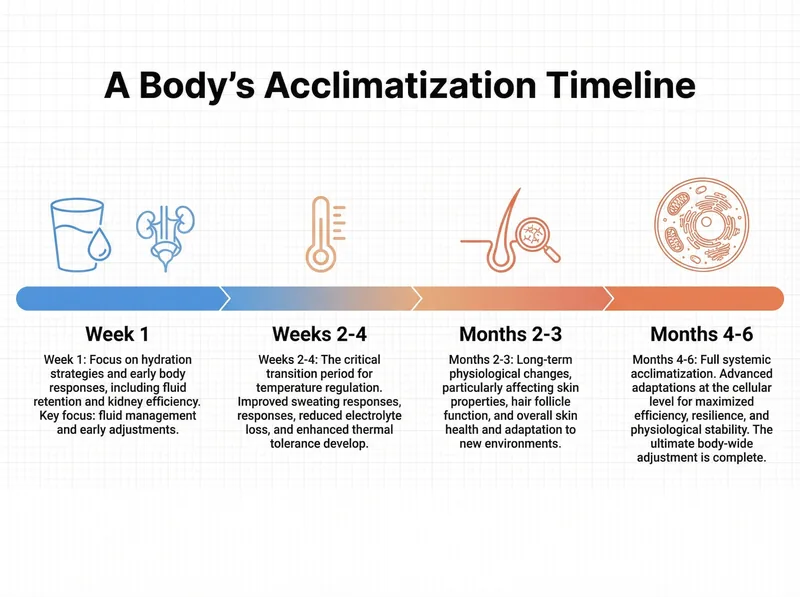 Your body’s adaptation timeline: what changes when during climate acclimatisation
Your body’s adaptation timeline: what changes when during climate acclimatisation
What Actually Happens to Your Body When You Relocate
Your body operates within a narrow range of acceptable internal conditions. Temperature, pH balance, hydration status, electrolyte concentrations, all of these have to stay within specific parameters for your cells to function properly. When you move from a temperate climate to extreme heat, or from soft water to hard water, you’re asking your body to maintain those same internal conditions while the external environment has shifted dramatically.
The technical term is homeostatic stress. Your body can absolutely adapt, but the adaptation process requires energy, time, and often additional nutritional support. Research on heat acclimatisation shows that it takes 10-14 days for your cardiovascular system to adjust to consistent heat exposure and 4-6 months for full physiological adaptation across all body systems.
But here’s what makes relocation particularly challenging: you’re not just adapting to one environmental change. You’re adapting to heat, humidity (or lack thereof), different water chemistry, altered UV exposure, new air quality, and often significant lifestyle changes all at once. Each of these creates its own set of physiological demands.
The result? Your body prioritizes survival functions first. Temperature regulation gets top priority. Hydration maintenance is critical. Everything else, hair growth, skin cell turnover, even some aspects of immune function, gets temporarily downregulated while your body figures out how to function in the new normal. This isn’t dysfunction. It’s a completely rational biological response to environmental stress.
The Hydration Crisis No One Warns You About
You’ve probably heard you need to drink more water in hot climates. What you haven’t heard is that your fluid needs can increase by 50-100% depending on the temperature differential and your activity level. If you were drinking 2 liters a day in a temperate climate, you might need 3-4 liters in extreme heat just to maintain baseline hydration.
The problem isn’t just volume. It’s absorption and retention. When you sweat heavily, you lose electrolytes, primarily sodium, but also potassium, magnesium, and calcium. Studies on exercise in heat show that sweat rates can reach 1-2 liters per hour in extreme conditions, and that sweat contains 900-1000mg of sodium per liter.
If you’re replacing that fluid loss with plain water, you’re diluting your electrolyte concentrations further. Your body can’t hold onto water without adequate sodium. This is why you can drink constantly and still feel dehydrated, the water isn’t staying in your system long enough to hydrate your cells.
Then there’s the water quality issue. Hard water in Gulf regions contains high concentrations of dissolved minerals, primarily calcium and magnesium. While these aren’t harmful to drink, they can affect how your body processes hydration. Some people report feeling less satisfied by hard water, drinking less as a result, and entering a chronic mild dehydration state that affects everything from sleep quality to hair health.
The fix isn’t complicated, but it requires intention. You need more water, yes. But you also need adequate electrolytes to retain that water. This means either adding a quality electrolyte supplement to your routine or ensuring your diet includes sufficient sodium and potassium. And if the local water quality is affecting your intake, investing in a filtration system or switching to bottled water with a lower mineral content can make a measurable difference in how hydrated you actually feel.
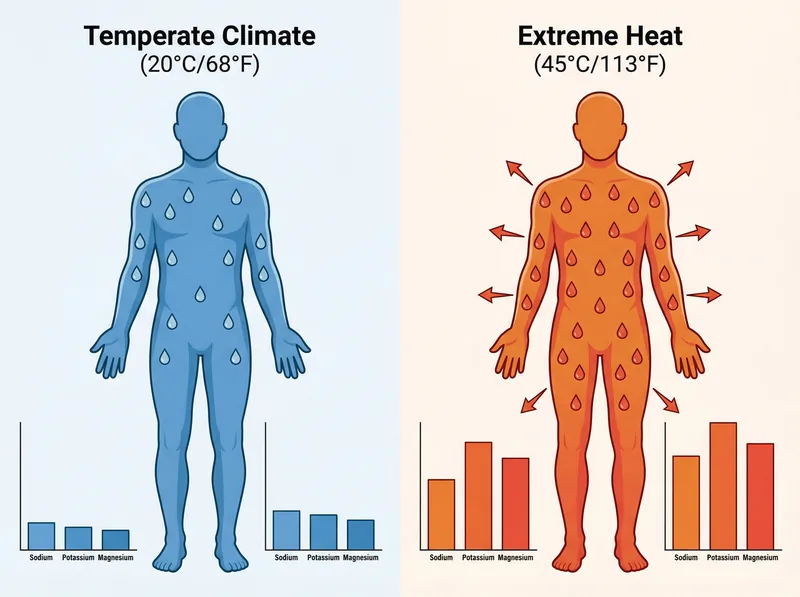 How extreme heat changes your body’s hydration needs: the science of increased fluid loss
How extreme heat changes your body’s hydration needs: the science of increased fluid loss
Temperature Regulation and Energy Depletion
Your body maintains a core temperature of approximately 37°C (98.6°F) regardless of the external environment. In temperate climates, this happens passively most of the time. In extreme heat, it requires active, energy-intensive cooling mechanisms running constantly.
Sweating is the primary cooling method, but it’s metabolically expensive. Your cardiovascular system has to increase blood flow to your skin to facilitate heat dissipation. Your heart rate increases even at rest. Research from Mayo Clinic indicates that prolonged heat exposure can improve resting heart rate by 10-20 beats per minute during the adaptation period.
This is why you feel exhausted in the first few weeks. Your body is burning significantly more energy just maintaining basic temperature regulation. It’s like running a low-grade fever, except the heat source is external. You’re not sick, but you feel depleted because your metabolic demands have increased substantially.
The adaptation process involves your body becoming more efficient at cooling. Your sweat glands become more active and start producing sweat at lower temperature thresholds. Your blood plasma volume increases to support better circulation. But these adaptations take time, typically 10-14 days for cardiovascular changes and up to 6 weeks for full thermoregulatory efficiency.
During this adaptation window, you need more rest than usual. Your sleep requirements might increase by an hour or more. Your appetite might decrease because digestion generates heat. And you’ll need to be more strategic about when you’re active. Early morning or evening activities become essential rather than optional because your body simply can’t handle midday heat exposure while it’s still adapting.
Hair, Skin, and the Hard Water Factor
If your hair texture has changed or your skin feels perpetually dry, the culprit is likely the local water chemistry. Hard water contains high concentrations of calcium and magnesium salts. When you wash with it, these minerals deposit on your hair shaft and skin surface, creating a barrier that prevents moisture absorption.
On hair, this manifests as mineral buildup that makes strands feel rough, look dull, and resist styling. On skin, it changes your natural lipid barrier, leading to increased transepidermal water loss. You moisturize, but the moisture can’t penetrate the mineral film. The result is skin that feels tight and dry no matter how much product you apply.
The combination of hard water and low humidity creates a perfect storm for barrier damage. In temperate climates with soft water, your skin and hair maintain their protective barriers relatively easily. In dry, hard water climates, those barriers are under constant assault. Your moisturizer stops working not because the product changed, but because the mineral deposits prevent it from reaching your skin.
For hair, the solution involves regular clarifying with a chelating shampoo like Regrowth+ that specifically removes mineral buildup rather than just surface oils. For skin, it means switching to gentler cleansers that don’t further strip your compromised barrier and layering hydrating products in a specific order, humectants first to draw water in, then occlusives to seal it.
Some people invest in whole-house water softening systems. Others install shower filters. The effectiveness varies depending on the specific mineral content in your area, but any reduction in mineral exposure helps. The key is recognizing that this isn’t a personal care failure. It’s an environmental factor that requires an environmental solution.
 Your climate adaptation support kit: practical tools that help your body adjust faster
Your climate adaptation support kit: practical tools that help your body adjust faster
Hormonal Shifts and Stress Response
Relocation triggers a measurable stress response in your body, and that stress affects your hormonal balance. Cortisol, your primary stress hormone, increases during the adaptation period. This isn’t just psychological stress from the life change. It’s physiological stress from the environmental demands your body is managing.
Improved cortisol affects everything. It changes your sleep-wake cycle, making it harder to fall asleep and stay asleep. It can trigger telogen effluvium, a form of stress-related hair loss that typically appears 2-3 months after the stressor begins. It affects your appetite, your digestion, and your immune function.
For women, the hormonal changeion can extend to menstrual cycle changes. Some experience irregular periods in the first few months after relocating. Others notice changes in PMS symptoms or cycle length. Research on circadian changeion shows that significant environmental changes can temporarily affect reproductive hormone regulation.
The adaptation here is partly time, your body will eventually recalibrate, but you can support the process. Maintaining consistent sleep and wake times helps reset your circadian rhythm faster. Managing psychological stress through whatever methods work for you (exercise, meditation, social connection) reduces the overall cortisol load. And ensuring adequate nutrition, particularly B vitamins and magnesium, supports your body’s stress response pathways.
If you’re experiencing significant hair loss or menstrual irregularities that persist beyond 3-4 months, it’s worth consulting a healthcare provider. Most relocation-related hormonal changeion resolves within six months, but persistent symptoms might indicate an underlying issue that needs attention.
Nutrient Depletion and Supplementation Strategy
Your increased metabolic demands in a hot climate create higher requirements for several key nutrients. You’re losing water-soluble vitamins (B complex, vitamin C) through increased sweat production. Your body’s using more magnesium and potassium for muscle function and electrolyte balance. And if you’re spending less time outdoors due to heat avoidance, your vitamin D synthesis might actually decrease despite living in a sunny climate.
This is the counterintuitive reality: vitamin D deficiency is surprisingly common in sun-heavy regions because people spend most of their time indoors in air conditioning. When outdoor temperatures regularly exceed 40°C (104°F), midday sun exposure becomes dangerous, and the times when it’s safe to be outside (early morning, evening) are when UV intensity is lower.
The nutrient that gets depleted fastest is sodium, but it’s also the easiest to replace through diet. The more concerning depletions are magnesium, potassium, and B vitamins because these affect everything from energy production to hair growth to sleep quality. Iron status can also decline in women, particularly if menstrual irregularities are causing heavier periods.
A strategic supplementation approach during your first 6-12 months can make a substantial difference. At minimum, consider a quality B-complex, magnesium (glycinate or threonate forms for better absorption), and vitamin D3 with K2. If you’re experiencing significant fatigue or hair changes, getting your iron and ferritin levels checked is worthwhile. A complete supplement stack for Gulf conditions addresses these common deficiencies systematically.
But supplements are support, not substitutes. Your foundation is still diet. Prioritizing whole foods, adequate protein, and a variety of colorful vegetables ensures you’re getting the full spectrum of nutrients your body needs for adaptation. Think of supplements as insurance against the gaps that environmental stress creates, not as a replacement for proper nutrition.
Sleep Changeion and Recovery
Sleep problems are nearly universal in the first few months after relocating to a hot climate. Your circadian rhythm is regulated partly by temperature, your body temperature naturally drops in the evening as a sleep signal. In consistently hot environments, that temperature drop is harder to achieve, and your sleep-wake cycle gets confused.
Air conditioning helps, but it creates its own issues. The dry air can irritate your respiratory system and skin. The temperature differential between indoors and outdoors can be 20-30°C, and moving between these extremes multiple times a day is physiologically taxing. Your body never quite knows what temperature environment to prepare for.
Then there’s the light exposure issue. Long summer days with intense sunlight affect melatonin production. If you’re getting bright light exposure late into the evening (which is common when outdoor activities shift to evening hours to avoid daytime heat), your melatonin onset gets delayed. You don’t feel sleepy until much later, but you still need to wake up at a reasonable hour, and chronic sleep restriction accumulates.
The solution requires environmental improvation. Your bedroom needs to be genuinely cool, 18-20°C (64-68°F) is ideal for sleep. Blackout curtains are essential, not optional, because any light exposure during sleep hours affects sleep quality. And you might need to be more intentional about evening wind-down routines because the natural temperature and light cues your body relies on are absent.
If sleep problems persist beyond the first few months, it’s worth investigating whether chronic mild dehydration is playing a role. Dehydration affects sleep quality, and many people don’t realize they’re consistently under-hydrated because they’ve adapted to the sensation. Ensuring adequate fluid and electrolyte intake, particularly in the evening, can improve sleep substantially.
Building Your Personal Adaptation Protocol
The adaptation timeline varies by individual, but most people see significant improvement by month three and feel fully adjusted by month six. You can’t speed up the biological processes, but you can support them and reduce the severity of symptoms during the transition.
Start with hydration as your foundation. Calculate your fluid needs based on your body weight and activity level, then add 50% for heat exposure. Track your intake for a few days to see if you’re actually hitting that target. Most people aren’t. Add electrolytes, either through a quality supplement or by being more liberal with salt in your diet.
Address the water quality issue directly. Whether that’s installing a shower filter, using a chelating shampoo weekly, or switching to bottled water for drinking, reducing your mineral exposure makes a measurable difference in how your skin and hair respond. This isn’t vanity. Barrier function affects your overall comfort and hydration status.
Improve your sleep environment aggressively. Blackout curtains, cool temperature, consistent schedule. If you’re struggling with sleep despite these measures, consider whether evening light exposure (screens, bright indoor lighting) is delaying your melatonin onset. Blue light blocking glasses or apps can help, but the most effective solution is simply dimming lights and reducing screen time in the two hours before bed.
Give yourself permission to rest more during the adaptation period. Your body is working harder than usual just to maintain basic function. This isn’t the time to push through fatigue or maintain the same activity level you had in your previous climate. Listen to your body’s signals and adjust accordingly. The adaptation will happen faster if you’re not fighting it.
References
- Heat Acclimatization and Cardiovascular Adaptation in Humans - National Center for Biotechnology Information
- Fluid Balance and Electrolyte Loss During Exercise in Heat - PubMed Central
- Heat Exhaustion: Symptoms and Causes - Mayo Clinic
- Circadian Rhythm Changeion and Hormonal Changes - PubMed Central
- Thermoregulation and Human Performance in Hot Environments - National Institutes of Health
